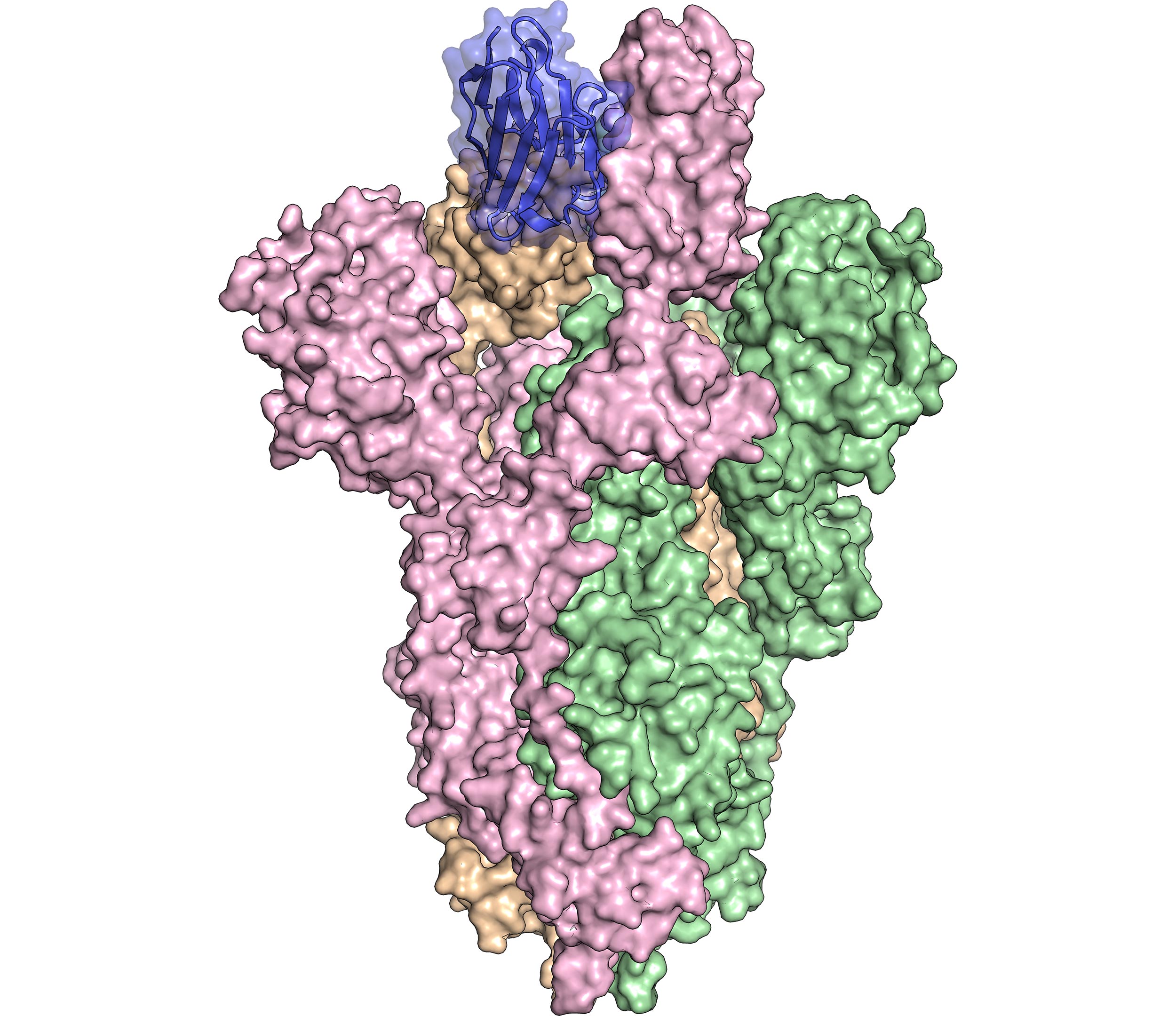 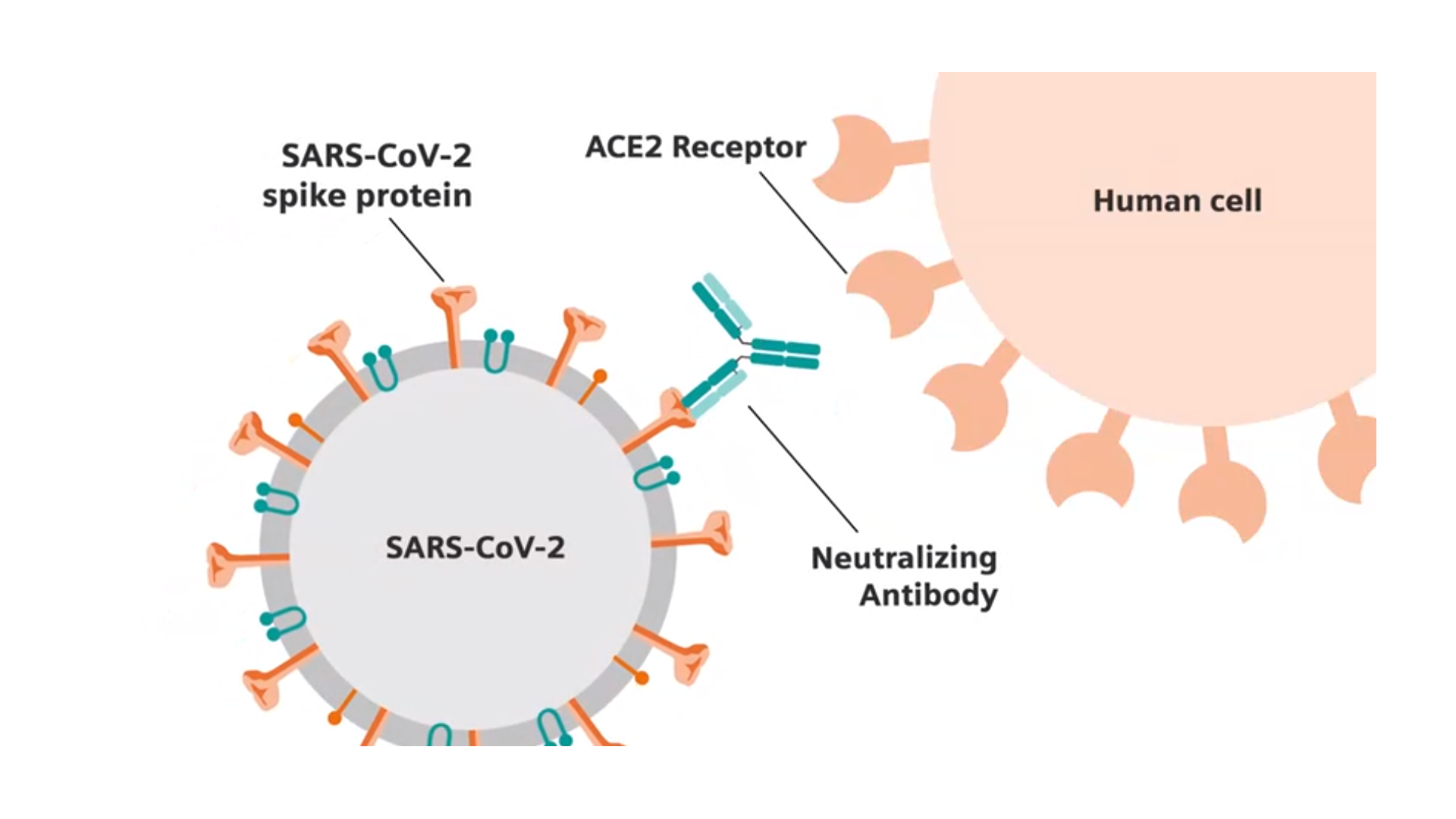
Serum remnants were retrieved from blood samples collected for routine laboratory testing during hospitalization and aliquots were stored at −80 ☌ before analysis. RT-PCRs for detection of SARS-CoV-2 RNA in nasopharyngeal swab samples were performed using the Allplex 2019-nCoV Real-time PCR (Seegene, Seoul, Korea), PowerChek 2019-nCoV (KogeneBiotech, Seoul, Korea), or Real-Q 2019-nCoV Real-Time Detection (BioSewoom, Seoul, Korea) detection kits according to respective manufacturer instructions. All patients were confirmed COVID-19 positive by RT-PCR between March 2020 and December 2020 at Seoul St. We collected a total of 191 serial serum samples from 32 COVID-19 patients (16 males, 16 females, median age 63 years (range 35–83 years). We also assessed time-course antibody responses according to disease severity and its correlation with neutralizing antibody results from sVNT. The aim of this study was to evaluate and compare early SARS-CoV-2 S protein antibody responses of COVID-19 patients using three fully automated quantitative chemiluminescent immunoassays (CLIAs): Architect SARS-CoV-2 IgG II Quant (Abbott, Chicago, IL, USA), Elecsys Anti-SARS-CoV-2 S (Roche, Basel, Switzerland), and Atellica IM SARS-CoV-2 IgG (sCOVG) (Siemens, Munich, Germany). To date, limited data are available correlating quantitative SARS-CoV-2 S protein antibody responses with sVNT results. The SARS-CoV-2 surrogate virus neutralization test (sVNT) (GenScript, Netherlands) is currently available for detecting neutralizing antibodies targeting the RBD based on antibody-mediated blockage of the interaction between the ACE2 receptor and SARS-CoV-2 RBD. With the widespread use of vaccines and therapeutics, longitudinal detection and quantification of antibody responses associated with neutralization becomes increasingly important. Antibodies to S protein and RBD can produce a potent virus neutralizing response by inhibiting virus binding to the host ACE2 receptor. Infection is mediated by interaction of the SARS-CoV-2 S protein RBD with the angiotensin converting enzyme 2 (ACE2) S1 subunit viral receptor on host cells. However, there are a limited number of studies evaluating quantitative S protein antibody levels after COVID-19 infection. Quantitative detection may be useful to assist interpretation of COVID-19 immunity and to evaluate active immunization. Recently, quantitative serologic assays for measuring antibodies against the receptor binding domain (RBD) of the S protein have been developed. Several studies have already compared some of these assays and found acceptable concordance. Most serologic assays are qualitative and use either nucleocapsid (N) or spike (S) SARS-CoV-2 protein as the target for antibody detection. To date, many SARS-CoV-2 antibody assays have been developed with different antigen targets and assay formats. Accurate antibody measurements support uncertain identification or evaluation in the case of resolved infection and can be useful for contact tracing and epidemiologic studies. Further standardization and harmonization of immunoassays might be helpful in monitoring immune status after COVID-19 infection or vaccination.Ĭoronavirus disease 2019 (COVID-19), caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), has become a pandemic and presents a major health concern across the globe. SARS-CoV-2 S protein antibody levels as assessed by the CLIAs were not interchangeable, but showed reliable performance for predicting sVNT results. CLIAs had good performance in predicting sVNT positivity (Area Under the Curve (AUC), 0.959–0.987), with Abbott having the highest AUC value ( p < 0.05). However, Passing–Bablok regression analysis showed significant proportional differences between assays and converting results to binding antibody units (BAU)/mL still showed substantial bias. Antibody levels from the three CLIAs were correlated (r = 0.763–0.885). When we assessed time-course antibody levels, the Abbott and Siemens assays showed higher levels in patients with severe disease ( p < 0.05). All assays detected >90% of samples collected 14 days after symptom onset (Abbott 97.4%, Roche 96.2%, Siemens 92.3%, and GenScript 96.2%), and overall agreement among the four assays was 91.1% to 96.3%. We compared the results of three chemiluminescent immunoassays (CLIAs) (Abbott, Roche, Siemens) and a surrogate virus neutralization test (sVNT, GenScript) using 191 sequential samples from 32 COVID-19 patients. Quantitative SARS-CoV-2 antibody assays against the spike (S) protein are useful for monitoring immune response after infection or vaccination.
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
